Why Can’t I Lose Weight? The Science Behind Weight Loss Resistance
Many people who struggle with weight loss ask the same question: “Why can’t I lose weight, even when I try?”
The answer is not always as simple as eating less or exercising more. For many patients, weight loss resistance is influenced by metabolism, hormones, insulin response, appetite regulation, sleep, stress, and long-term biological adaptation.
Understanding these factors can help patients stop blaming themselves and start looking at weight management as a medical process, not just a matter of willpower.

What Is Weight Loss Resistance?
Weight loss resistance refers to difficulty losing weight despite consistent efforts with diet, exercise, or lifestyle changes. It does not mean that weight loss is impossible. It means that the body may be responding in ways that make the process slower, harder, or less predictable.
For some people, this may be related to insulin resistance. For others, hunger hormones, metabolic adaptation, sleep problems, stress, or underlying health conditions may play a role. In many cases, several factors are involved at the same time.
This is why a personalized medical evaluation is important before choosing any weight loss treatment.
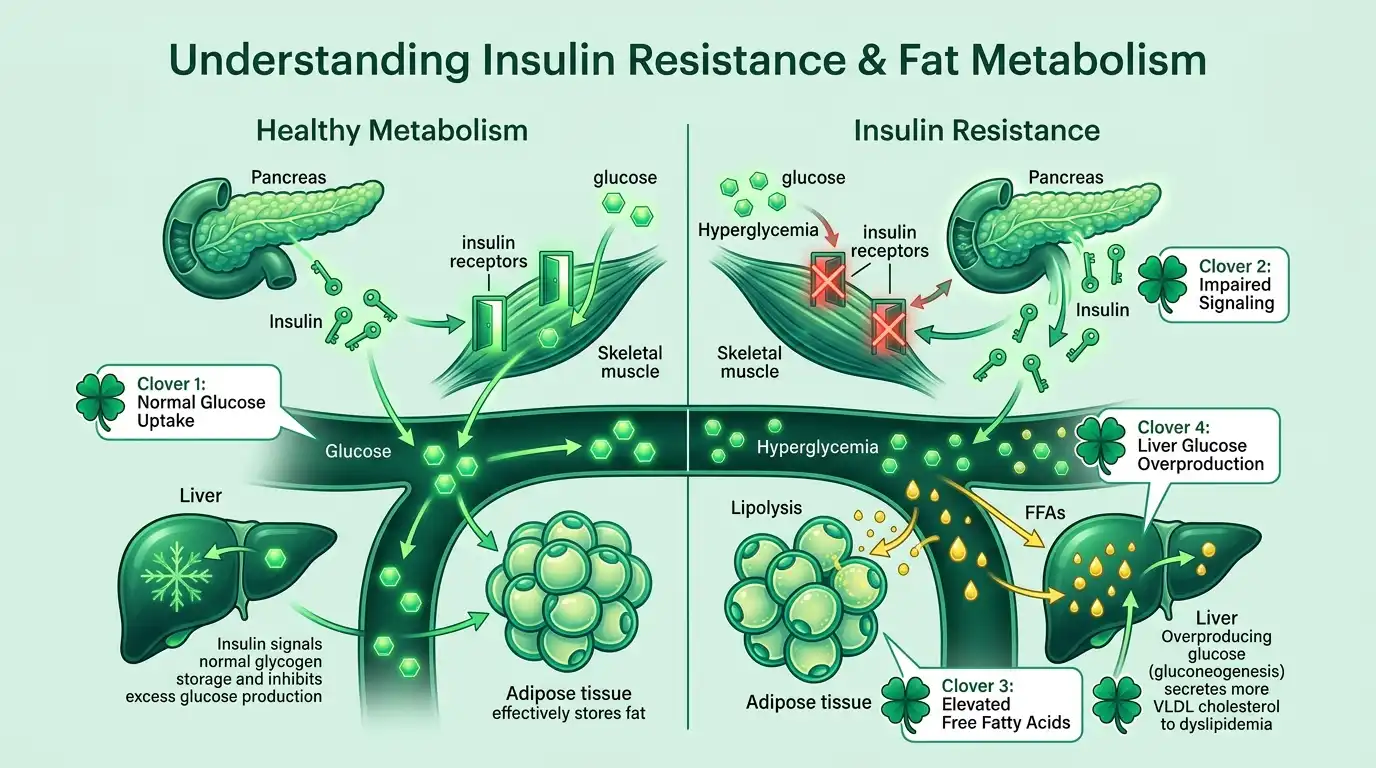
Insulin Resistance: A Common Barrier to Weight Loss
Insulin is a hormone that helps move sugar from the blood into the cells, where it can be used for energy. When the body becomes resistant to insulin, cells do not respond to it as effectively. As a result, blood sugar levels may rise, and the body may need to produce more insulin to keep things under control.
Insulin resistance is common in people with obesity, but it does not affect everyone in the same way. It can make weight management more difficult by influencing hunger, fat storage, energy levels, and the risk of developing type 2 diabetes.
This is one reason why doctors often look beyond weight alone. Blood sugar levels, insulin response, metabolic health, and obesity-related conditions are all important parts of the evaluation.
Your Body Defends Its Weight
One of the most frustrating parts of weight loss is that the body often reacts as if weight loss is a threat. When you lose weight, your body may try to conserve energy and increase hunger.
This is called metabolic adaptation. During weight loss, the body may reduce overall energy expenditure, while appetite-related hormones also change. Research shows that weight loss can be associated with lower leptin levels, higher ghrelin levels, and reduced energy expenditure, all of which can make continued weight loss more difficult.
In simple terms, your body may burn fewer calories than before while also making you feel hungrier. This is one reason why diets often work in the short term but become harder to maintain over time.

Hunger Hormones: Leptin, Ghrelin, and GLP-1
Weight loss is strongly influenced by hormones that control appetite and fullness.
Ghrelin is often called the “hunger hormone” because it increases appetite. Leptin is produced by fat tissue and helps signal fullness and energy availability. GLP-1 is produced mainly in the gut and helps regulate appetite, insulin secretion, and fullness after meals.
When these signals are disrupted, patients may feel hungry even after eating, struggle with cravings, or find it difficult to stay satisfied with smaller portions. This does not mean the patient lacks discipline. It means the body’s appetite regulation system may be working against long-term weight loss.
Why Diets Often Fail Long-Term
Many diets create an initial calorie deficit, which can lead to early weight loss. However, over time, the body adapts. Hunger increases, metabolism slows, and daily energy expenditure may decrease.
This is why many patients experience a cycle of losing weight, hitting a plateau, becoming frustrated, and then regaining weight. The problem is not always the diet itself; it is the body’s biological response to weight loss.
![]()
For patients with obesity, sustainable weight loss often requires more than temporary restriction. It may require medical guidance, metabolic evaluation, behavioral support, and in some cases, medications or bariatric surgery.
When Should You Consider Medical Support?
You may benefit from medical evaluation if you:
- struggle to lose weight despite repeated diet attempts
- regain weight after losing it
- have insulin resistance, prediabetes, or type 2 diabetes
- experience constant hunger or strong cravings
- have obesity-related conditions such as sleep apnea, hypertension, or joint pain
A medical evaluation can help identify what is actually driving weight gain or weight loss resistance. The goal is not to follow another generic diet, but to choose the right approach for your body.
Treatment Is Not One-Size-Fits-All
Some patients may benefit from lifestyle changes and nutritional guidance. Others may require medical treatment, weight loss medications, or bariatric surgery depending on their BMI, metabolic health, medical history, and long-term goals.
The right treatment plan should always be personalized. What works for one patient may not be suitable for another.
At BB Global Health, the focus is on understanding the full picture: metabolism, hormones, eating patterns, medical history, and obesity-related health risks. This allows patients to receive a treatment plan based on their individual needs, not trends or guesswork.



